The Evidence-Informed Decision Making (EIDM) Casebook Issue 3
This issue was published in 2019 and includes six stories from Canadian and international public health professionals that demonstrate the use of evidence-informed decision making (EIDM) in a wide range of public health activities, either using evidence to inform a program or intervention, or building capacity for EIDM. The stories describe the initiatives, implementation, evaluation, and lessons learned from using evidence in practice, or building capacity for EIDM.
Download PDF version.
Click here to explore the other issues of the EIDM Casebook.
Access slides and recordings from presentations in the NCCMT’s Peer-to-peer webinar series, featuring authors of stories from the third issue of the EIDM Casebook.
Featured Stories
Dr. Mridula Bandyopadhyay and Dr. Milica Markovic
Department of Health and Human Services, Victoria, Australia
Newborn bloodspot screening is an important tool to screen for rare and serious medical conditions. Read more about how the Department of Health and Human Services in Victoria, Australia, implemented a quality improvement project aiming to increase the use of newborn bloodspot screening and to meet key performance indicators.
Jane Murrell
City of Hamilton Public Health
Facing an outbreak of raccoon strain rabies, the City of Hamilton and the Ministry of Natural Resources and Forestry created and implemented a rabies prevention and control initiative. Read more about how this innovative public awareness campaign was developed and implemented to promote awareness of rabies.
Maja Bertram, Natasa Loncarevic, Arja R. Aro
Department of Public Health, Unit for Health Promotion Research, University of Southern Denmark
In order to build capacity and experience in intersectoral evidence-informed policy making, researchers undertook a project that spanned multiple countries. Read more about how the REPOPA project used innovative strategies to study as well as build experience and knowledge in evidence-informed policy making, using evidence from various contexts.
Becky Hester, Diana Miller, Caitlyn Paget, Chetna Pandya
York Region Public Health
Prior to 2018, food handler certification was not mandatory in Ontario. As such, some municipalities developed their own bylaws. Read more about how the Regional Municipality of York explored and implemented a bylaw in their region mandating food handler certification for food premises.
Dr. Cheryl Cusack,1 Michelle Johnson,2 Jan Schmalenberg,1
1Manitoba Health, Seniors, and Active Living – Population & Public Health Branch, 2Prairie Mountain Health Authority
Before 2013, there were no national public health nurse competencies for prenatal, postpartum and early childhood periods. Read more about how Manitoba Health, Seniors, and Active Living developed and implemented standards for prenatal, postpartum, and early childhood public health nurses to address this gap.
Dr. Drona Rasali and Daniel Fong
British Columbia Centre for Disease Control, Provincial Health Services Authority
The Population and Public Health team at the BC Centre for Disease Control undertook a project to support the integration of data into the community health planning process in British Columbia. Read more about the creation and implementation of the Community Health Data website and its associated resources.
Full Text Stories
Newborn bloodspot screening practice in Victoria: Australian experience
Department of Health and Human Services, Victoria, Australia
Background and Rationale
The first 1000 days of life are critical for the health and well-being of all children. This time between conception and the second birthday provides a unique opportunity to lay the foundation for optimal health outcomes across the lifespan. One way to promote a healthy start to life is through newborn bloodspot and neonatal hearing screening, both of which occur during these first 1000 days.
Bloodspot screening, which is the focus of this case study, is one of the most successful public health programs in Australia. Nurses and midwives collect bloodspots (four droplets of blood) on a special card from a newborn’s heel 48 to 72 hours after birth, air dry it for four hours and then send it to a statewide laboratory for screening. This procedure is a quick, safe and effective way to identify newborns at risk of having rare but serious medical conditions, including physical and intellectual disabilities. Early identification allows for early interventions in the first few weeks of life, which can prevent adverse health outcomes and promote health and well-being across the lifespan.
Objectives
According to the Australian evidence-based newborn bloodspot screening guidelines, bloodspot samples should be collected 48 to 72 hours after birth and reach the laboratory within 96 hours (four days) of collection to enable early interventions to prevent adverse outcomes. The quality of the sample is also important to avoid repeat sampling. This includes ensuring the cards are dried properly and there is no sample contamination. A public health approach requires that any gap between the guidelines and practice be addressed through a quality improvement initiative.
Initiative
The purpose of the initiative in Victoria, Australia, was to identify maternity service providers not meeting key performance indicators, conduct site visits and facilitate quality improvement. The targets of the initiative were public and private maternity health services and independently practicing private midwives. Data on the timeliness of sample collection and dispatch/transport (time to reach the state laboratory from collection) between January 1, 2017 and December 31, 2017 for each maternity service provider were analyzed to establish a baseline. The data were also used to monitor and track the improvement of each maternity service provider in Victoria in achieving the recommended collection and timeliness standards.
Over a 12-month period beginning March 1, 2018, the maternity services with the longest times between sample collection and dispatch were selected for a site visit to identify barriers in providing a high-quality newborn bloodspot screening program. These visits enhanced understanding of a number of local issues related to:
- geography and remoteness;
- network and the availability of domiciliary midwives;
- pathology courier services and postal services; and
- individual hospital policy and practice, including their impact on providing high-quality service.
The next phase of the intervention targeted maternity services performing in the mid-range. The last phase focused on visits with the best-performing maternity services to understand their systems and processes for providing a high-quality newborn bloodspot screening program.
To improve the timeliness and sample quality of the lower-performing maternity services, we collaboratively tailored and developed an individual action plan with the maternity provider, key stakeholders such as the pathology service providers and their courier services, to find local solutions to local problems. Other collaborative initiatives to encourage excellence in newborn bloodspot screening included universal interventions, such as:
- promoting participation in free online education for midwives, nurses and maternity administrative staff;
- designing a user-friendly flyer on the newborn bloodspot screening process for midwives; and
- developing a newborn bloodspot screening poster for consumers and nursing and midwifery health professionals.
Multimedia tools were also developed to aid and facilitate seamless sample collection and dispatch to improve performance. These tools included a video on the lived experience of an Australian parent whose child was diagnosed with phenylketonuria and a virtual tour of the screening laboratory. The latter video aimed to enhance understanding of what happens to the collected bloodspot samples at the screening laboratory, including sample processing, sample retention and research.
Universal interventions were complemented by provider-specific targeted interventions, such as holding interactive regional workshops and involving local patients with the lived experience of being diagnosed with a rare disease through newborn bloodspot screening and its ramifications. These workshops included problem solving based on real case scenarios elicited through site visits.

Forums were held in the capital city, Melbourne, for public and private hospitals and independently practising private midwives to bring together specialist clinicians and midwives. The attendees highly valued these opportunities to discuss the importance of a high-quality screening program and its impact on newborns’ lives.
Evaluation and Impact
The midwives and nurses attending the capacity-building training evaluated it as 100% satisfactory. They felt that they improved their knowledge and understanding of the newborn bloodspot screening program, and learned correct methods for sample collection, drying and dispatch. They also formed lasting networks with other maternity service providers. The development of the initiative in consultation with key stakeholders played a significant role in how well the initiative was received and the level of enthusiasm surrounding implementation. Since the beginning of the initiative, performance indicator improvements have been observed across the board. Data for the first quarter of 2019 show an overall increase in timeliness in bloodspot sample collection at the state level, including at the public hospital sector, which is the largest maternity service provider in Victoria.
The implemented initiatives are self-sustaining. Momentum is expected to continue as these initiatives are system-wide and process-based. Since staff turn-over and leadership changes may potentially slow down the quality of performance, performance will continue to be monitored quarterly, and additional interventions may be implemented if needed.
Lessons Learned
One key lesson learned from this experience was that data are an important first step for driving quality improvement. Data informed one-on-one, face-to-face engagement with maternity service providers to understand their challenges and develop solutions collaboratively. A key factor in successfully implementing the identified initiatives was taking into account the specific context of each maternity service provider. For example, ownership and buy-in of the initiatives were much greater when they were jointly organized. Involving maternity providers’ senior leadership in developing a local action plan was also essential to the success of this intervention.
"Knowing they are able to prevent life-long disability...gives staff a sense of purpose in making a positive difference in a newborn's life and motivation to continue to provide a high-quality program to save lives"
The rarity of conditions identified through newborn bloodspot screening means that the majority of staff have never come across a newborn with any of the screened conditions. Meeting children and family members at interactive workshops allowed maternity providers to experience the real impact of the newborn bloodspot screening program on long-term health and social outcomes. Knowing they are able to prevent life-long disability by correctly collecting four bloodspots and dispatching them on time gives staff a sense of purpose in making a positive difference in a newborn’s life and motivation to continue to provide a high-quality program to save lives.
Back to Top.
Rabies is Real campaign – Using evidence-based results to widen Rabies awareness in Hamilton
City of Hamilton Public Health Services
Background and Rationale
December 4, 2015 marked the first report received by Hamilton Public Health Services in Ontario of a rabid raccoon testing positive for the raccoon strain of the virus. It had been involved in an attack on two dogs. The raccoon was the first terrestrial animal to be infected with the virus in Hamilton since 1994. The situation quickly progressed to the largest raccoon strain rabies outbreak in Canadian history, involving multiple regions and municipalities. To date, 462 animals have tested positive for rabies, with 332 of these from Hamilton. A rabies prevention and control initiative by the Ministry of Natural Resources and Forestry in partnership with the City of Hamilton Public Health Services was initiated with the goal of eradicating raccoon rabies from the Hamilton area. First steps involved updating rabies-awareness materials and creating a new public awareness campaign.
Objective
The goal of the new rabies awareness campaign was to “grab attention” and prevent future exposures. The intent of the campaign design was to drive residents to the city’s website for more information.
Initiative
A marketing company was contracted to create the campaign. Two styles were provided for consideration (see image 1 and 2). The first was a typical health education piece with a picture of a raccoon. The second style was a creative combination of rabies vector species using a bat, raccoon, skunk and fox to create hybrid animals called the “Baccoon” and “Skox.” Focus group testing was conducted using the two campaign ideas. Participants included internal staff, members of the public, pet owners, children and non-English speaking residents. People were surveyed at various locations including dog parks, an international centre, other city departments and a children’s day camp. The focus group testing was kept simple and involved showing participants both posters and asking them to select the one they liked most and indicate why. Participants were also asked, “Which poster would most likely get your attention and potentially create conversation?”

Results indicated the “Baccoon” poster was the favourite, selected by 84% of the participants. They provided descriptive comments, including, “it’s different and eye catching,” “it might trigger questions because it’s weird” and “it’s more likely to be shared on social media.” Five of the thirteen individuals who chose the other poster changed their minds when asked the question, “Which poster would most likely get your attention and therefore create conversation?” Most non-English-speaking residents also selected the “Baccoon” poster. They thought the raccoon in the other poster was a dog, while the hybrid image using a bat caused them to question what the poster was about because it looked strange to them. In addition, the results indicated considerable variability in the level of rabies awareness across participants.
Implementation
The “Baccoon” and “Skox” images were selected for the “Rabies Is Real” campaign, which officially launched city-wide in September 2016. The campaign consisted of billboards, posters in bus transit stations, vehicle wraps on two Animal Services vehicles, posters in arenas and city buildings and social media ads (see image 2). The campaign was also shared with other health units and key partners. To date, three other health units have adopted the campaign for their own rabies education programs. In addition, the Ontario Association of Veterinarian Technicians used the images for their “Protect Your Pet” campaign in 2017 and 2018.
Evaluation and Impact
To measure the success and outreach of the campaign, a convenience sampling evaluation was completed in 2018 using both online and hard copy surveys. The objectives of the evaluation were to:
- determine the reach of the awareness campaign; and
- determine the level of knowledge of rabies for residents of the City of Hamilton.
Summary of Evaluation
- A total of 2,369 completed entries.
- Most respondents (93.8%) had heard about rabies prior to this survey, and of those who had, 77% knew about rabies within the City of Hamilton.
- Just over half of respondents (52.9%) were able to identify the “Baccoon” or “Skox” ads and the key health messages conveyed through these ads.
- 84% of respondents identified cats as potential vectors of rabies compared to 93% identifying dogs and 97% identifying raccoons.
- 82% of respondents responded correctly when asked about rabies wound care.
- Most respondents (82%) responded correctly when asked if rabies is fatal.
- Some respondents (26%) thought that birds were a vector species of rabies.
Results of the evaluation revealed that more efforts were needed to focus on cats being a potential vector species. Given that Hamilton has already seen two rabid stray cats since the outbreak started, this became a new program objective. The outcome was the creation of a new hybrid: a cat and dog called the “Purrpup” (see image 3). This image focused on domestic animals being at risk for rabies and was also more appropriate for rabies education at veterinary clinics where the public could relate the messaging to pets.
Lessons Learned
Sharing the creative work with other health units and partners has broadened the impact and reach of this education campaign. A few challenges were encountered during its release. For example, when creating the names of the hybrid animals, it was decided to use quotation marks so there would be no issues when translating to other languages. After the campaign launched, it became known that the term “Skox” has an unfavourable urban dictionary meaning. This was unfortunate, however because the word “Skox” is always used with the image and the tagline “Rabies Is Real,” it was felt there would be no misunderstanding. The evaluation also showed some residents were unaware that rabies is fatal and proper wound care should be an essential first step for protection.
The evaluation indicated that these important points needed to be emphasized more on our posters to improve awareness. Moving forward, the following issues will require ongoing improvements to ensure improved community awareness about rabies:
- Ensure all health messaging includes and clearly states rabies can cause death.
- Dispel myths around which animals can and cannot transmit rabies.
- Continue to re-enforce health messaging when dealing with animal exposures.
- Continue to reiterate the importance of rabies prevention through animal vaccinations, avoidance of wild animals and supervision of pets.
"Fortunate unplanned outcomes included the image of the “Baccoon” transcending language barriers as many non-English-speaking residents recognized a bat but wanted to ask more questions when the image was combined with a raccoon."
Fortunate unplanned outcomes included the image of the “Baccoon” transcending language barriers as many non-English-speaking residents recognized a bat but wanted to ask more questions when the image was combined with a raccoon. This was not something considered prior to the design stage. The “Rabies Is Real” campaign has been popular on social media platforms due to its unique and eye-catching images. Overall, the evaluation demonstrated that the campaign successfully kept Hamilton residents safe from rabies, while also identifying additional ways to improve the campaign.
If you would like to access any of the resources discussed in this story, please contact Jane Murrell at jane.murrell@hamilton.ca.
Back to Top.
REsearch into POlicy to enhance Physical Activity (REPOPA)
Maja Bertram, Natasa Loncarevic, Arja R. Aro
Department of Public Health, Unit for Health Promotion Research, University of Southern Denmark
Background and Rationale
There is strong evidence for the health benefits of regular physical activity and how different physical environments influence active living. Research evidence can also be used to help build effective policies. However, there is still a need for more knowledge on how to integrate research evidence in health to enhance physical activity policies. These policies can be both direct physical activity policies and policies creating environments that support physical activity.
In an attempt to build experience and knowledge on how to improve intersectoral evidence-informed policy making about physical activity, the REPOPA project (REsearch into POlicy to enhance Physical Activity; www.repopa.eu) was launched. The European Union’s Seventh Framework Program funded the project, which took place from October 2011 to September 2016. REPOPA used an evidence-informed policy-making approach, where research evidence was integrated with additional sources of evidence from local contexts, resources and societal and political needs and preferences.
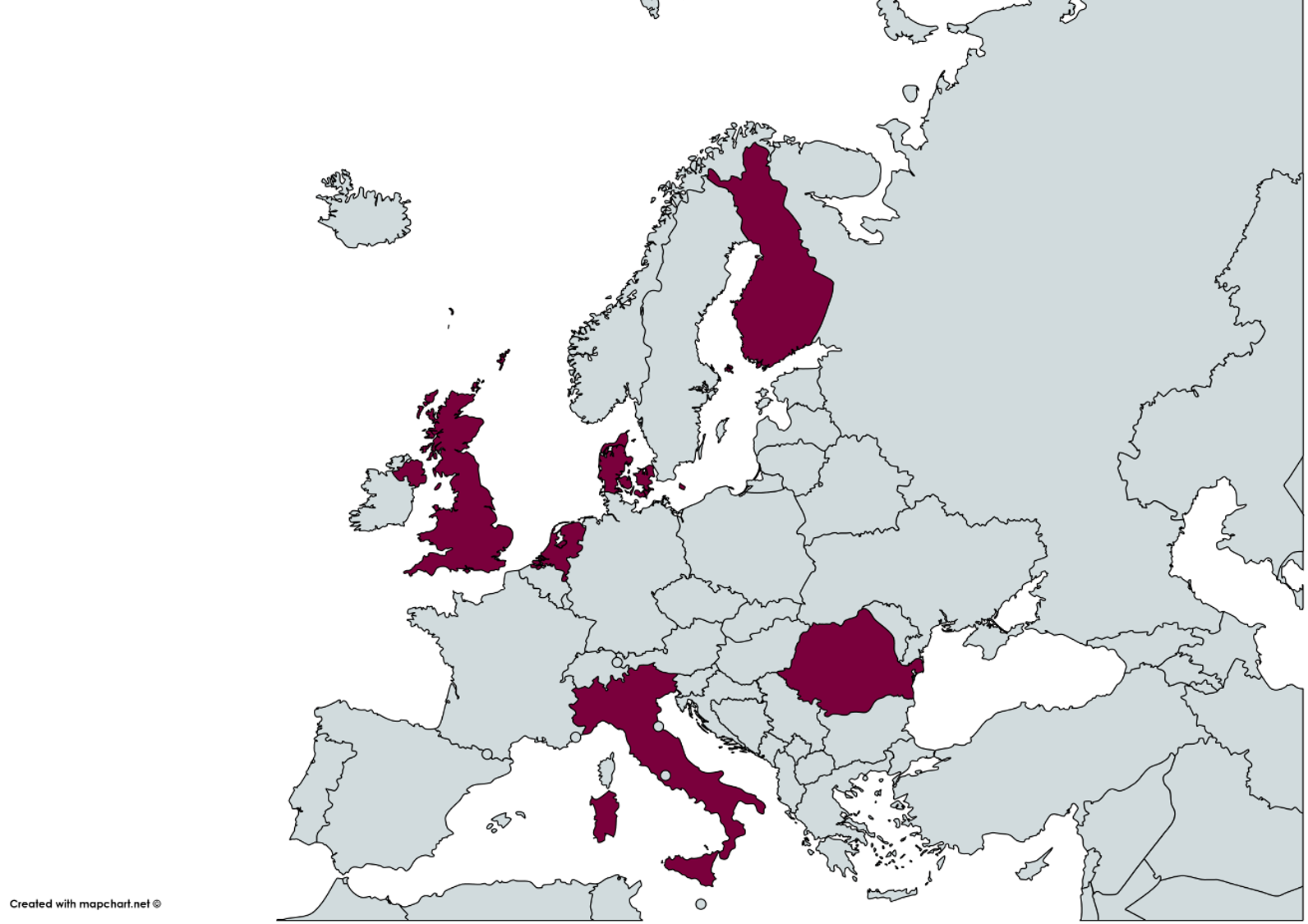
The project was carried out in six European Union countries (Denmark, Finland, Italy, the Netherlands, Romania and the United Kingdom), with Canada functioning as the project evaluation partner. The outcomes and results of the project can be useful in Canada when planning the development and implementation of policies in relation to physical activity or other health promotion activities.
Objectives
The objectives of the REPOPA project were to:
- study the status of research use and other types of evidence in physical activity policy making by document analysis and stakeholder interviews;
- study two types of physical activity policy-making interventions—policy games and locally tailored stewardship interventions—to increase evidence-informed policy making; and
- develop indicators to assess the level of evidence-informed policy making.
Initiative, Implementation, and Evaluation
REPOPA applied a programmatic design, meaning that each phase of the project informed the successive phases.
Phase 1
The project started with a thematic content analysis of 21 policies and interviews with policymakers and experts (n = 86). The main barriers for the use of research evidence in policy making were:
- traditions;
- bureaucratic and organizational factors;
- the nature of policy-making processes and political interests;
- lack of available or applicable research when needed;
- academic language being difficult for non-academics to understand; and
- lack of procedures to gather research evidence or to meet researchers.
Additional identified factors included lack of time, limited financial and human resources, and lack of competence and guidelines for the use of research evidence in the policy-making process.
The main facilitators for the use of research evidence in policy making were:
- support from administrative departments to use research evidence;
- an organizational culture that supports evidence-informed policy making;
- the availability of research that is relevant and feasible to implement in practice; and
- direct or institutional relationships between policymakers and researchers.
Phase 2
Based on Phase 1 findings, the project developed two types of interventions.
The first intervention was a policy game to stimulate the use of evidence in local policy making and enhance collaboration to increase mutual understanding between policymakers and different organizations (e.g., governmental organizations such as municipal departments and non-governmental organizations such as patient organizations and sport clubs). The policy game was carried out in the Netherlands, Denmark and Romania. The country teams designed the game, chose real policy cases, conducted a systems analysis and prepared the performance.
The policy games were designed based on a basic script: A fictitious municipality where different stakeholders were working on the implementation of a physical activity policy. The aim was to develop intersectoral interventions through collaboration between stakeholders and design an overall implementation plan that fits the aims of the physical activity policy. A game leader facilitated the game and made sure the script was followed. To develop integrated, intersectoral interventions, the teams in the game needed to get support from other teams. In the end, the game leader evaluated the result and, together with the accountable stakeholders in the game, decided whether the interventions proposed by the teams (which form the final implementation plan) met the objectives of the physical activity policy.
The policy games were adapted to local contexts and 18–20 participants per country took part. As an example, the policy game in Denmark was developed around a policy called “The Health policy 2013–16—a common affair in Elsinore.” The specified target group was all citizens in the municipality, with special attention on citizens with special needs and chronic diseases. The policy had a strong focus on physical activity promotion for all citizens, including children and youth. The aim of the policy was to develop surroundings in the municipality that gave equal opportunities for healthy living for all citizens. The game focused on making an implementation plan for this policy.
Data related to the experience of participating in the game were measured via observations and questionnaires administered before the games, immediately after the games ended and six months after the games. The policy games appeared to increase mutual understanding between the policymakers and organizations involved. They also demonstrated the importance of organizational and leadership support for using research evidence, especially in intersectoral collaboration. Furthermore, the games led to increased insight into policy processes, including organizational networks and stakeholder roles. There was also a positive change observed in the attitude and behaviour toward collaboration, aspects of leadership and use of evidence. In addition, the policy games helped illustrate the benefits of using expertise and various sources of evidence in the policy-making process.
The second intervention was a stewardship-based, locally tailored intervention based on needs, context and stakeholder analysis. Each country team in Denmark, Italy and the Netherlands selected two policy cases for their intervention. In Denmark, the intervention aimed to increase intersectoral collaboration and strategic policy making. In the Netherlands, the intervention aimed to strengthen physical activity planning. In Italy, the interventions focused on knowledge and research translation for two physical activity strategies. Interventions included workshops, training sessions, networking, knowledge exchange and consultation. The interventions lasted from six to 18 months. A questionnaire was carried out before, immediately after the intervention and 12-months post intervention.
The interventions proved to be useful for increasing the level of evidence-informed policy making and also improved access to, requests for and the use of research evidence. There was also a decrease in barriers for using research evidence, and politicians requested research evidence more often. While the evaluation demonstrated that needs-based interventions as well as collaborative policy making are an effective way to enhance evidence-informed policy making, the 12-month follow-up showed that it was challenging to sustain these effects in the longer term.
Phase 3
The results were validated and negotiated among the stakeholders from the participating countries and representatives from other EU countries using a Delphi method. The Delphi study produced a list of 25 measurable indicators for evidence-informed policy making and eight further complex indicators, which are not (yet) measurable. The 25 indicators consisted of four categories:
- Human resources – competences and networking
- Documentation – retrieval/production
- Communication and participation
- Monitoring and evaluation
The Delphi process was implemented in three stages: two Internet-based Delphi rounds at the international level (76 participants) and a third face-to-face Delphi stage at the national level in the six REPOPA countries. The final 25 measurable indicators can be used as a policy-making checklist to assess if and the extent to which the policy in question is evidence-informed. Please see Development of measurable indicators to enhance public health evidence-informed policy making for further information on these indicators. Evidence briefs and fact sheets were also developed to summarize the evidence gathered from each of the six country settings. All material can be found on the REPOPA webpage.
Lessons Learned
The REPOPA project identified several ways in which researchers could help policymakers support evidence-informed policy making:
- Communicate the results of available, relevant and feasible research without using academic jargon.
- Build processes and mechanisms to gather research evidence as well as meet and build relationships with policymakers.
- Use policy games to increase mutual understanding between policymakers and researchers.
- Emphasize the importance of organizational and leadership collaboration across sectors.
“These locally tailored interventions helped policymakers take into account the needs and values of the people for whom the policies were directed, as well as encouraging them to request research evidence more often.”
REPOPA researchers also joined real-world physical activity policy groups and helped them use research evidence. These locally tailored interventions helped policymakers take into account the needs and values of the people for whom the policies were directed, as well as encouraging them to request research evidence more often. REPOPA was not only an academic project; it also developed the findings into usable tools such as indicators for evidence-informed policy making.
REPOPA used physical activity as the theme in its work; however, the lessons learned and tools developed can be applied to other fields, especially in the area of healthy living.
Back to Top.
Promoting evidence-based food handler legislation in York Region
Becky Hester, Diana Miller, Caitlyn Paget, Chetna Pandya
York Region Public Health
Background and Rationale
In 2018, food handler certification (FHC) became mandatory in Ontario, joining other provinces and municipalities that require food premises to have staff on-site who are trained in safe food handling. A food premises is anywhere that food for public consumption is prepared or served, including restaurants but also mobile food trucks, food production plants, snack bars, cafeterias, serveries in hospitals and long-term care facilities, and more.
Before 2018, Ontario required public health units (PHUs) to ensure that training was locally available and to encourage food premises to employ certified food handlers. However, hiring certified food handlers was voluntary unless a municipality had passed a mandatory FHC bylaw. Jurisdictions with FHC bylaws prior to 2018 included Toronto, Niagara, Hamilton and London.
Objectives
In 2015, before mandatory province-wide FHC, York Region Public Health (YRPH) considered whether to pass a local FHC bylaw. The bylaw’s aim was to increase the number and proportion of food premises with certified staff, with the intention of increasing safe food handling practices and improving premises’ compliance at public health inspections.
“The bylaw’s aim was to increase the number and proportion of food premises with certified staff, with the intention of increasing safe food handling practices and improving premises’ compliance at public health inspections.”
The project team considered multiple issues in the development of an FHC bylaw, including:
- whether or not to pass a bylaw;
- the contents of the bylaw (e.g., whether to require certified staff at all premises or only higher-risk premises, how many certified staff to require and whether to require owner/operators to be certified); and
- how to implement and enforce the bylaw (e.g., how to inform operators and monitor compliance, and whether to phase in enforcement).
Assessing the Evidence for Mandatory Food Handler Certification
YRPH considered multiple sources of evidence to decide whether to pursue a bylaw. A comprehensive literature review indicated that food safety training improves knowledge and attitudes toward food safety. The literature search strategy focused on combinations of different keywords to represent the concepts of food handling or food inspection; certification or education or bylaw; public health; and mandatory. The search was performed in databases for academic literature and through a Google search, supplemented by hand searching of PHUs and agencies for grey literature. Of the 70 articles found, three systematic reviews and one grey literature report were deemed to be relevant and of strong methodological quality.
To assess local attitudes toward certified food handling, YRPH surveyed over 1,000 York Region residents and found that 88% supported a bylaw. This survey consisted of a custom module about public support for FHC legislation added to the 2014 Rapid Risk Factor Surveillance System, a representative telephone survey of Ontario residents conducted annually by select Ontario PHUs.
YRPH also analyzed original data on the effectiveness of FHC. The food safety program added questions on FHC to routine public health inspection forms. As a result, public health inspectors (PHIs) collected information from every inspected food premises about whether anyone was certified, who was certified (e.g., a food handler vs. an owner/operator) and whether the certified person was on-site during the inspection. This data collection allowed YRPH to analyze four years of inspection records (2011–2014). The results demonstrated that premises with certified staff had fewer infractions and complaints, along with fewer enforcement activities (e.g., orders, closures, tickets).
Because FHC was found to be an evidence-informed intervention with widespread public support, YRPH decided to pursue a mandatory FHC bylaw.
Using Evidence to Inform the Bylaw Contents
The content of FHC legislation across jurisdictions varies in terms of who must be certified (e.g., owner/operators or food handlers, one food handler or multiple) and whether a certified person must be on-site at all times. YRPH’s analysis of inspection records found that having a certified food handler on-site was more effective than having one on staff, and that having a certified owner/operator on staff (although not necessarily on-site) was particularly associated with increased compliance. Accordingly, the York Region bylaw required a certified owner/operator on staff and a certified food handler on-site during all operating hours.
Implementation
YRPH took a phased-in approach to enforcement with earlier implementation for premises with a higher risk rating. FHC was required at high-risk premises beginning in 2017 and at moderate-risk premises beginning in 2019. Health units assign each food premises a risk rating based on standardized criteria provided by the Ministry of Health and Long-Term Care, including complexity and extent of food handling, type of population served and compliance history. These factors are weighted and calculated to determine each premise’s minimum frequency of inspections per year.
High-risk premises were identified as a priority due to the increased risk to the public and the increased frequency of inspections (three per year, compared to two for moderate-risk premises). This gave PHIs more opportunities to educate operators on the bylaw before enforcement began.
YRPH launched a targeted communication campaign to inform owners/operators of the bylaw. This campaign included multiple components:
- Stakeholder meetings with owners/operators to educate them on bylaw requirements and answer their concerns
- Emails, letters and postcards sent to each food premise to inform them of the bylaw
- Separate reminder emails and letters sent to high- and moderate-risk premises as enforcement began
- One-on-one education for owners/operators provided by PHIs during inspections

- Meetings with municipal bylaw officers to educate them on bylaw requirements
- Advertisements placed in local papers to inform the general public about the bylaw
- Updating of the YRPH website to inform owners/operators and the public about the bylaw
YRPH also offered additional FHC workshops to accommodate the increased demand for certification.
The bylaw was monitored and enforced by PHIs during routine inspections, with a focus on supporting owners/operators during the phase-in periods through education and consultation rather than ticketing and enforcement. PHIs educated owners/operators on the new bylaw and helped them register their staff for food handler workshops. These in-person educational services were complemented by post-card mail outs and other targeted communications based on monitoring of the bylaw status at all premises. Although the bylaw allowed PHIs to ticket premises for non-compliance, only one ticket was issued under the bylaw in 2017, the first year the bylaw was enforced.
Impact
The bylaw increased the proportion of food premises with a certified food handler on-site. In 2016, 45% of high-risk food premises and 47% of all food premises had certified staff on-site; by 2017, 71% of high-risk food premises and 55% of all premises had certified staff on-site. Even though enforcement had not yet begun at moderate-risk premises, the proportion of moderate-risk premises with a certified food handler on-site increased as well.
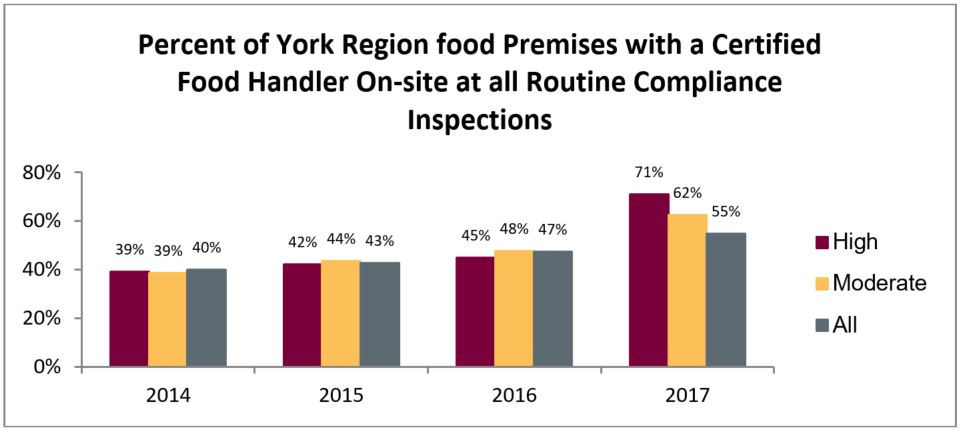
Local municipalities’ bylaws, including the York Region bylaw, may have contributed to the province adopting mandatory FHC. The case of food handler certification illustrates how local evidence-informed legislation can pave the way for broader (provincial), systemic legislative change.
Lessons Learned
For other jurisdictions considering the creation and implementation of local bylaws, we recommend our approach of breaking down a complex change into multiple decision points. This allows the most relevant sources of evidence to be considered for each decision. Additionally, the use of multiple sources of evidence can assist in tailoring the information needed for the different stakeholders of each stepwise decision point.
Phased-in enforcement and a focus on outreach and education with owners/operators were also instrumental in obtaining compliance. This parallels YRPH’s comprehensive, education-based approach to public health inspections. Although our work focused on the impact of mandatory FHC in food premises, the approach is relevant to jurisdictions considering other forms of mandatory training in other settings, such as recreational water facilities or businesses inspected for infection prevention like daycares or personal services, to support widespread improvement in public health practices.
Back to top.
The development and implementation of standards in prenatal, postpartum and early childhood public health nurse practice in Manitoba
Dr. Cheryl Cusack,1 Michelle Johnson,2 Jan Schmalenberg1
1Manitoba Health, Seniors and Active Living – Population & Public Health Branch, 2Prairie Mountain Health Authority
Background and Rationale
Competency-based standards specific to the public health nurse (PHN) role in the prenatal, postpartum and early childhood periods did not exist in Canada in 2013. Concurrently, national experts identified role clarity and the development of a common vision based on the full scope of practice as a priority.(1) To address this issue, Manitoba developed provincial PHN standards and launched them in 2015. These provincial standards built upon national standards and competencies for PHN practice (2) (3) and therefore may be of broad interest.
Objective(s)
The short-term objective of this initiative was to articulate consistent and measurable activities for PHN roles in prenatal, postpartum and early childhood practice. Standards represent “a vision for excellence” and articulate measurable PHN benchmarks.(2) The Manitoba standards aim to depict the full scope of the PHN role in promoting healthy early childhood development and health equity within a population-based practice. The long-term goal was development of tools and resources to support implementation and attainment of the standards by all PHNs in the province.
“Standards represent “a vision for excellence” and articulate measurable PHN benchmarks.”(2)
An important first step at the outset of the initiative was to distinguish between population health, primary health care and primary care. To work to full scope in a population-based practice, PHNs must understand the distinctions between these concepts and be deliberate when making daily clinical decisions.
- Population health was defined as encompassing multiple strategies with the goal of advancing the health of populations and reducing inequities among population groups.(4)
- Primary health care was defined as an approach to transform health services and improve health status based on principles of health promotion and disease prevention, accessibility, public participation, appropriate technology and intersectoral collaboration.(5)
- Primary care was defined as health care services delivered in community-based settings.(5)
Universal PHN programs and services apply systematic methods to identify individuals not well-connected to traditional systems who would benefit from focused PHN intervention and follow-up. Conversely, individuals who are knowledgeable and capable of accessing primary care are referred there by PHNs for their health care services.
Initiative
The National Collaborating Centre for Methods and Tools’ (NCCMT) model for evidence-informed decision making (EIDM) guided the process of developing and implementing the standards. According to the model, EIDM is informed by multiple sources of evidence including public health expertise, local community health issues, public health resources, community and political climate, and research.(6) As the foundation for evidence-based practice, research was highlighted under each heading.
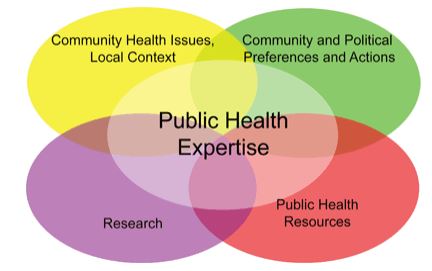
Data were collected on multiple items within each of these broad areas of EIDM. For instance, the local community health sections highlighted Manitoba population demographics, geography, cultural attributes and perinatal health outcomes. The public health resources section incorporated national standards,(2) competencies,(3) roles and activities (7) for public health nursing, and focused on opportunities for PHN interventions to advance health equity in Manitoba. The community and political climate sections summarized specific Manitoba legislation and service delivery models impacting PHN practice. Lastly, the research section summarized evidence regarding prenatal, postpartum, healthy child development and health equity.
Implementation
The final product from this initiative was the development of Manitoba standards, documentation forms, clinical pathways and webinars. Throughout the initiative, ministry staff worked in close collaboration with the regional health authorities as well as individual PHNs, which is considered to be a crucial component of the success of this initiative. Provincial public health leaders kept the standards and tools as routine monthly team agenda items, while staff, managers and directors participated in various committees that reviewed, piloted and adapted the tools based on PHN practice in Manitoba. Another crucial component of the initiative that ensured ongoing progress was the creation of a new project leadership term position at Manitoba Health, Seniors, and Active Living (MHSAL) from May 2013 to April 2016. An additional position was obtained in May 2017 to continue to advance and implement the standards.
The final implementation component was a series of webinars to disseminate information across the province. PHNs participated in the development of the webinars, which were held in August and September 2018. The first webinar provided the background and context, recognizing that the project had been ongoing for several years. The second webinar focused on prenatal, the third on postpartum and newborn, and the last on documentation forms and processes. Again, the EIDM model was used as a framework to guide the webinar content and development. The webinars were recorded and are available on the Manitoba Health website, along with the supporting documents. PHNs continue to access them and they are used in the orientation of new staff.

Evaluation and Impact
Before publication of the standards in 2015, survey data were gathered using a modified Delphi technique. The survey consisted of all of the standards statements followed by a five-point Likert scale. Participants were asked to rank their level of agreement with each statement and boxes were also provided for written text. The intent was to have three survey rounds to revise and gain consensus on standards statements with less than 70% agreement, however results after the first round found that 90% of participants agreed or strongly agreed with the majority of the statements. The few statements where levels of agreement were in the 80% range pertained to timing of follow-up. Comments in the text boxes reflected concern with the ability to meet the benchmarks with existing resources, as opposed to the content of the statements. As there were no statements with less than 70% agreement, subsequent rounds of the survey and revisions to the standards statements were not required.
The final method of evaluation took place during the webinars. During each of the four webinars, participants were asked via polling questions to gauge their readiness to implement the standards based on the ADKAR model.(8) The ADKAR model is a tool to guide change using a ranking scale that measures the stages of awareness, desire, knowledge, ability and reinforcement. Consistent with the earlier feedback, participants generally reported that they had the knowledge to implement the standards. Methods to evaluate the impact of standards in practice are under development.
Lessons Learned
The Manitoba Standards define minimum practice expectations for PHNs in the areas of prenatal, postpartum and early childhood. The process involved the collaboration of PHNs, nursing leaders, regional health authorities and MHSAL. Additional full-time MHSAL positions that were created specifically for this project were essential in providing leadership and maintaining momentum for this initiative. The level of engagement of PHNs and regional leadership was critical to project success and organizational change management, and contributed measurably to the smooth implementation of the tools into practice.
References
- Schofield, R., Ganann, R., Brooks, S., McGugan, J., Dalla Bona, K., Betker, C. et al. (2011). Community health nursing vision for 2020: Shaping the future. Western Journal of Nursing Research, 33(8), 1047-1068.
- Community Health Nurses of Canada. (2019). Canadian Community Health Nursing Professional Practice Model & Standards of Practice. Ottawa, ON: Community Health Nurses of Canada.
- Community Health Nurses of Canada. (2009). Public Health Nursing Discipline Specific Competencies. Ottawa, ON: Community Health Nurses of Canada.
- Government of Canada. (2012). Key Elements and Actions that Define a Population Health Approach. Ottawa, ON: Health Canada.
- Canadian Nurses Association. (2015). Primary Health Care: CNA Position. Ottawa, ON : Canadian Nurses Association.
- National Collaborating Centre for Methods and Tools. (revised 2012). Evidence-Informed Public Health: A Model For Evidence-Informed Decision-Making in Public Health [fact sheet]. Retrieved from https://www.nccmt.ca/uploads/media/media/0001/01/d9f5cec8637db62f8edda6a6a2551b293a053ede.pdf.
- Canadian Public Health Association. (2010). Public Health ~ Community Health Nursing Practice in Canada. Roles and Activities (4th ed.). Ottawa, ON: Canadian Public Health Association.
- Prosci. (n.d.). What is the ADKAR Model? Retrieved from https://www.prosci.com/adkar/adkar-model
Back to top.
Community health data website: Driven by the local needs in British Columbia
British Columbia Centre for Disease Control, Provincial Health Services Authority
Contributors to this project:
Dr. Drona Rasali (since 2012), Bethany Elliot (2012–2016), Rita Zhang (2013–2018), Jesse Veenstra (2015–2016), Danielle Burch (2018–2019), Irene Ingel (2018–2019), Svetlana Ristovski-Slijepcevic (since 2017), Crystal Li (occasional, 2016–2019), Laili Qiyam (since 2019), Sarah Gustin (2013–2017), Ellen Lo (2018), Daniel Fong (since 2017) and PHSA Web Solutions Team led by Michael Zalter (since 2014).
Background and Rationale
Although British Columbia (BC) is one of the healthiest provinces in Canada, segments of its population struggle to achieve good health. There is a need to share health data to better understand and improve the health and well-being of these communities. This case describes an initiative to provide relevant data for evidence-based decision making in community health planning in BC. This initiative was driven by the health data needs of the provincial, regional and local governments, especially for reducing the growing burden of chronic disease through prevention and health promotion strategies.
Objectives
The main objectives of the project were to produce and provide a web-based platform to share readily usable and standardized data for community health planning across the province. The online community health data platform includes a variety of demographic, socioeconomic and population health status indicators.
Initiative
The Population and Public Health (PPH) team at the BC Centre for Disease Control (BCCDC), part of the Provincial Health Services Authority (PHSA), developed the Community Health Data website. The following online resources are included on the website:
- BC Community Health Atlas maps numerous health indicators for BC’s 131 municipalities (2013).
- BC Community Health Profiles (CHPs) use a common template to summarize standard community health indicator data. These were initially released for 131 major incorporated municipalities (2014), and then further improved and released as an interactive web tool for all 142 incorporated municipalities (2016).
- A searchable health database provides data for all indicators included in the CHPs, along with data for many other indicators of community health outcomes (2016).

The goal of the online resources is to help local governments, school boards and non-governmental organizations (NGOs) in evidence-based decision making for community health planning. The resources enable users to access, explore and use local data related to demographics, population health status and other factors that affect health. PHSA developed all resources in partnership with the BC Ministry of Health (MoH), five regional health authorities (Interior Health, Fraser Health, Vancouver Coastal Health, Vancouver Island Health and Northern Health), local governments (Union of BC Municipalities) and NGOs (BC Healthy Communities Society). Information specific to Indigenous peoples is not included in the current community health data resources due to lack of readily accessible data. There is a need to explore this further, working closely with the First Nations Health Authority.
Development and Implementation
As mandated by BC Healthy Communities, a provincial initiative for health promotion, PHSA initiated the project in 2012 and launched a province-wide Community Health Atlas in 2013, working collaboratively with BC Stats, DataBC and the Vancouver Island Health Authority.
Based on the strength of this work, the provincial initiative’s Healthy Communities Working Group further determined that community-specific health profiles were necessary to sufficiently meet local data needs for community health planning. PHSA thus developed CHPs for 131 incorporated municipalities in BC and released them on the PHSA website in 2014 in static PDF versions.
Shortly after, PHSA and the working group began exploring various options to make the profiles interactive, understandable and readily usable for informing local health planning. PHSA developed and packaged the online resources into three main components and made them accessible publicly in 2016 through the online platform of the BC Community Health Data website. Since 2016, the BC Observatory for Population and Public Health has been an integral partner in this project disseminating the online resources through its hub website ‘Quick Links’.
The searchable database includes data for a substantial number of indicators gathered from a variety of sources, including:
- demographics (10 indicators);
- social and economic factors (18 indicators);
- educational outcomes (8 indicators);
- general health (24 indicators) and student health (60 indicators);
- health behaviours (6 indicators);
- early childhood development (6 indicators);
- health systems (3 indicators);
- maternal/infant health (2 indicators);
- premature mortality (5 indicators); and
- cancer (9 indicators).
The working group selected a number of these indicators for inclusion in the CHPs through consensus. The indicators are organized into individual CHPs for all 142 incorporated municipalities in BC, and include uniform and consistent messaging describing the community-specific characteristics. About 20 smaller villages were excluded from the database due to lack of feasibility for data reporting.
In April 2019, the three online resources were updated with the latest available data. All three resources will be updated once newer data become available (e.g., after 2021 Census cycle).
Evaluation
Data from the Community Health Data website are widely used by local governments (e.g., Squamish City), medical practitioners (e.g., BC Guidelines: Primary Care of Diabetes), academic institutions (e.g., University of British Columbia, University of Victoria, Columbia Basin Institute), Public Health Association of BC, NGOs (e.g., PlanH), local news media and community media (e.g., Lake Country Calendar) to support evidence-informed program planning and decision making. A provincial evaluation of the BC Healthy Communities initiative conducted in 2014–2016 found that the CHPs and associated tools were perceived as resources that promote engagement of regional health authorities with local governments, meeting one of the goals of the province’s Healthy Communities Initiative.
The PPH team commissioned an evaluation in 2018–2019 to assess the effectiveness of the three community health data resources as well as the website platform that hosts the resources. An external consulting firm (Context Research) conducted surveys (n = 111), focus groups (n = 14) and interviews (n = 8) with local government staff members and regional health authority representatives, including medical health officers. The consulting firm also used web analytics for the three online resources. The findings from the evaluation indicated that the tools and resources provide valuable data and information for local communities, staff training and the general public.
“The findings from the evaluation indicated that the tools and resources provide valuable data and information for local communities, staff training and the general public.”
At the same time, the majority of the respondents expressed the need for more detailed community health information and data. The increased use of local data resulted in the need for improved profiles for newly formed local areas called Community Health Service Areas (CHSAs). Moreover, the interest shown by individuals other than the target stakeholders in using the online resources for knowledge transfer can be seen as a spin-off effect of the impact of these resources beyond the scope of community health planning.
Conclusions and Lessons Learned
This successful collaborative initiative focused on supporting evidence-based decision making in community health planning that is driven by the needs of local communities across BC. The resources developed by PHSA are an example of a collaboration that has progressively improved the availability of increasingly detailed local data since 2012. It offers new ways of sharing data through better visualization of ways to meet the needs of the end-users. The key to this project’s success lies in the process of ongoing engagement with stakeholders to determine what data is useful to collect (now and in the future), as well as sustaining the tools through dedicated efforts to maintain and update the resources.
In the process of developing these online resources, we uncovered gaps in data availability and refined our understanding of what data are useful to local communities. We also faced the challenge of tailoring and disseminating large amounts of data to make them user-friendly and useful for local needs. This project has provided insight into how data resources intersect, supplement and complement other community-specific profiles developed by Statistics Canada, the MoH and regional health authorities.
Stakeholders continue to want more detailed local data. When this project started, BC’s local health areas were the smallest geographic health boundary where data were commonly available and reportable; we now know this is not sufficiently detailed. The MoH has developed smaller geographic health boundaries (CHSAs), which will serve as new and more robust representations of local communities. Creating and re-envisioning community health data profiles at this new geographic level will help meet the data needs of local governments. In addition, the more-detailed data made available at the CHSA level of geography may facilitate integration of the data needs of public health as well as primary care networks, which were consulted while designing the new boundaries.
Back to top.